What Is Squamous Cell Carcinoma (SCC)?
Understanding SCC
What Is Squamous Cell Carcinoma?
Squamous cell carcinoma is a type of skin cancer that develops in the squamous cells — the flat cells that make up the outer layer of the skin. Around 23,000 new cases are diagnosed in the UK each year, making it the second most common skin cancer after basal cell carcinoma.
SCC grows faster than BCC and carries a small but real risk of spreading to other parts of the body if left untreated. Early assessment and treatment by a specialist is therefore particularly important.
SCC most commonly appears on sun-exposed areas of the body, including:
- The face, particularly the lips and ears
- The neck and scalp
- The hands and forearms
- Areas of previously damaged or scarred skin
Key Takeaways
- Squamous cell carcinoma is the second most common skin cancer in the UK, with around 23,000 new cases diagnosed every year
- SCC is more aggressive than BCC and carries a small but real risk of spreading, with around 2 to 5% of cases metastasising if left untreated
- The primary cause is long-term UV exposure, though HPV, chronic skin conditions, and a weakened immune system also increase risk
- Common signs include a firm red nodule, a scaly crusted patch, usually rapidly growing over a matter of weeks.
- Mohs micrographic surgery offers the highest cure rate of any SCC treatment, with cure rates of up to 97% for primary SCCs
- Miss Rakhee Nayar is one of fewer than 10 women in the UK dual-trained in plastic surgery and Mohs micrographic surgery, with over 20 years of experience and a 99.9% patient satisfaction rate
Knowing the Causes Can Help
What Causes Squamous Cell Carcinoma?
The primary cause of SCC is cumulative exposure to UV radiation from sunlight or sunbeds. Over time, UV damage to the DNA in squamous cells can cause them to grow in an uncontrolled way.
Other factors that increase your risk include:
- Fair skin, light eyes, or light hair — less natural protection against UV radiation
- A history of sunburn — particularly in childhood or early adulthood
- Sunbed use — artificial UV radiation carries the same risks as sunlight
- Pre-existing actinic keratoses or Bowen's disease — these are considered pre-cancerous conditions that can progress to SCC
- Human papillomavirus (HPV) infection — particularly associated with SCC on the genitals, lips, and inside the mouth
- A weakened immune system — including patients on long-term immunosuppressant medication
- A personal or family history of skin cancer
- Chronic skin inflammation or scarring — SCC can develop within long-standing wounds, scars, or areas of persistent skin inflammation

Request an e-Consultation
Speak with Miss Rakhee Nayar from the comfort of your own home and receive expert advice on your skin concern, treatment options, and next steps.

Spotting the Early Warning Signs
Who Is Most at Risk of Developing SCC?
SCC is most commonly diagnosed in adults over 50, and is more common in men than women. However, it can affect anyone, and cases in younger adults are increasing.
You may be at higher risk if you:
Have previously been diagnosed with actinic keratoses or Bowen’s disease
Have a weakened immune system — organ transplant recipients are at particularly high risk and may develop more aggressive SCCs
Have previously had an SCC — the risk of developing a second is significantly higher
Work or have worked outdoors for an extended period
What Are the Symptoms of Squamous Cell Carcinoma?
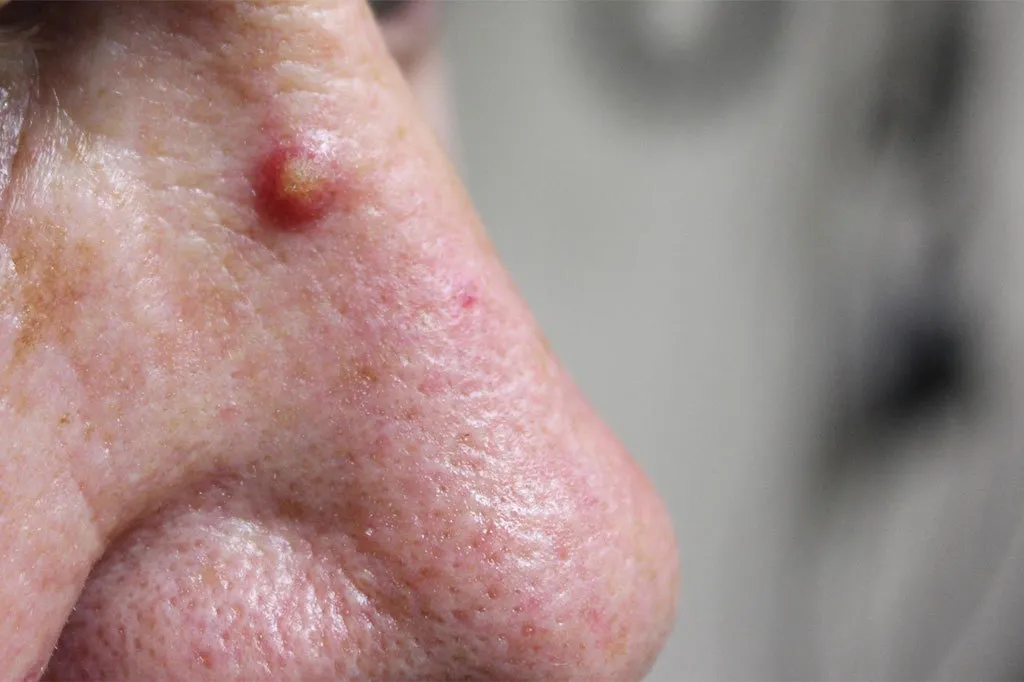
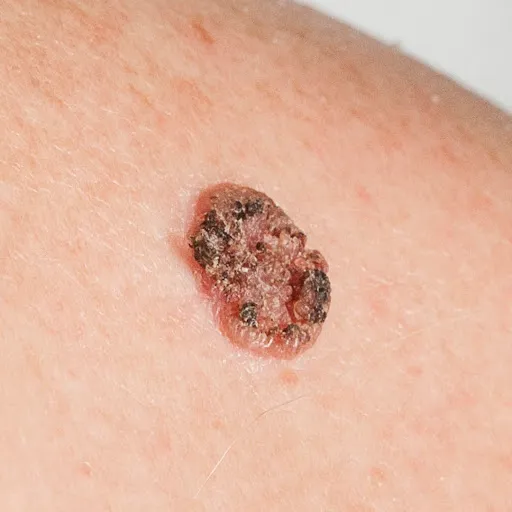
SCC often develops from a pre-existing rough or scaly skin patch. Unlike BCC, it can sometimes be tender or painful. Common signs to look out for:
- A firm, red nodule or raised lump on the skin
- A flat, scaly patch with a rough or crusted surface
- A wart-like growth that bleeds or crusts repeatedly
- A new sore or raised area within an existing scar
- A sore that does not heal
A Simple Skin Check Guide
ABCDE Checklist
When checking your skin, the ABCDE checklist is a useful guide for identifying lesions that warrant a specialist opinion. If a lesion on your skin meets any of these criteria, do not wait to see if it resolves on its own. Book a specialist assessment as soon as possible:
Border: the edges of the lesion are irregular, ragged, notched, or poorly defined. A clearly outlined, smooth border is generally a reassuring sign.
Diameter: whilst SCCs can vary in size, any lesion that is visibly growing warrants prompt attention, regardless of how small it may appear.
Evolution: any change in the lesion over time, including growth, a shift in colour or shape, or a new symptom such as bleeding, itching, crusting, or tenderness, should always be reviewed by a specialist.
How Serious Is SCC?
SCC is more aggressive than BCC but remains highly treatable when caught early. The key difference is that SCC carries a small but real risk of spreading to nearby lymph nodes and, in some cases, other organs — something that is extremely rare with BCC.
The most important thing to understand is that early treatment by an experienced specialist significantly reduces the risk of spread and leads to excellent long-term outcomes.
Around 2 to 5% of SCCs metastasise if left untreated. High-risk SCCs include those that are:
- Large or deeply invasive
- Located on the ears or lips
- Poorly differentiated under the microscope
- Arising within scars or areas of chronic inflammation
- Occurring in patients with a weakened immune system

How Is SCC Diagnosed?
If SCC is suspected, a specialist will carry out a clinical assessment and perform a skin biopsy to confirm the diagnosis. A small sample of tissue is removed from the lesion and examined under a microscope in a laboratory.
Results are typically available within one to two weeks. Unlike BCC, further imaging such as an ultrasound, CT scan or MRI scan, may sometimes be recommended to check whether the cancer has spread to nearby lymph nodes. Your specialist will advise whether this is necessary based on the characteristics of your lesion.
Prompt diagnosis is particularly important for SCC given its higher metastatic potential compared to BCC.
How Is Squamous Cell Carcinoma Treated?
Several treatment options are available for SCC. Your specialist will recommend the most appropriate approach based on the size, location, subtype, and depth of your tumour, as well as whether the cancer has spread.
Mohs Micrographic Surgery
The most precise and effective treatment for high-risk and facial SCCs, with cure rates of up to 97% for primary SCCs
Surgical Excision
Suitable for many SCCs in lower-risk locations
Curettage & Cautery
Used for small, superficial, low-risk SCCs
Radiotherapy
A non-surgical option for patients not suitable for surgery
Systematic Treatments
Immunotherapy or targeted therapy for advanced or metastatic SCC

Mohs Surgery for Squamous Cell Carcinoma
Mohs micrographic surgery is the most effective treatment for high-risk SCC, particularly for lesions on the face, ears, lips, and hands.
The tumour is removed layer by layer, with each layer examined under a microscope in real time until no cancer cells remain, ensuring complete removal whilst preserving as much healthy tissue as possible.
It is worth noting that Mohs surgery for SCC requires a surgeon with specific expertise in treating this cancer type. Miss Rakhee Nayar is one of the UK’s leading specialists in Mohs surgery for both BCC and SCC, and her European Hand Diploma makes her uniquely qualified to treat SCC on the hand whilst preserving maximum function.
Mohs surgery for SCC is particularly recommended when:
- The lesion is on the face, ears, lips, or hands
- The tumour is large, deeply invasive, or poorly differentiated
- The SCC has recurred following previous treatment
- The patient is immunocompromised
- The SCC has developed within a scar or area of chronic skin inflammation
Consultant Plastic Surgeon
Meet One of the UK's Leading Mohs Surgeons
Miss Rakhee Nayar is one of the UK’s foremost specialists in Mohs micrographic surgery, with particular expertise in the treatment of squamous cell carcinoma. In a specialty where only 17% of consultants are women, she offers a uniquely compassionate and relatable perspective valued by her patient base.
Can Squamous Cell Carcinoma Be Prevented?
Whilst not all SCCs can be prevented, the risk can be significantly reduced with consistent sun protection habits.
- Apply SPF 50+ sunscreen daily, even in winter or overcast weather
- Wear protective clothing and a wide-brimmed hat in strong sunlight
- Avoid sunbeds entirely
- Seek shade during peak UV hours between 11am and 3pm
- Have actinic keratoses treated promptly to prevent progression to SCC
- Check your skin regularly and seek prompt assessment of any new or changing lesions
Annual skin checks are strongly recommended for those in high-risk groups, particularly immunocompromised patients and those with a history of actinic keratoses or previous skin cancer.


07740 306144
Frequently Asked Questions
Common Questions About SCC
Is squamous cell carcinoma more dangerous than basal cell carcinoma?
SCC is generally considered more aggressive than BCC as it carries a higher risk of spreading to other parts of the body. However, when caught and treated early by a specialist, both types are highly treatable with excellent outcomes.
Can SCC spread to other parts of the body?
Yes, though it is relatively uncommon. Around 2 to 5% of SCCs metastasise if left untreated. High-risk SCCs — particularly those on the ears or lips, or in immunocompromised patients — carry a higher risk of spread. Early treatment significantly reduces this risk.
What is the difference between SCC and Bowen's disease?
Bowen’s disease is an early form of SCC that is confined to the outer layer of the skin and has not yet invaded deeper tissue. It is sometimes referred to as SCC in situ. If left untreated, Bowen’s disease can progress to invasive SCC, which is why prompt treatment is recommended.
How quickly does squamous cell carcinoma grow?
SCC generally grows faster than BCC, though the rate varies between individuals and subtypes. Poorly differentiated SCCs tend to grow and spread more quickly than well-differentiated ones. Any lesion that appears to be growing or changing should be assessed promptly.
Can SCC come back after treatment?
Recurrence is possible, particularly if the tumour was not fully removed during the initial procedure. Mohs micrographic surgery offers the lowest recurrence rates of any SCC treatment, with cure rates of up to 97% for primary SCCs.
What is the survival rate for squamous cell carcinoma?
When treated early, the survival rate for SCC is very high. The five-year survival rate for localised SCC is over 95%. The outlook is less favourable when the cancer has spread to the lymph nodes or other organs, which is why prompt specialist treatment is so important.
Can squamous cell carcinoma develop inside the mouth?
Yes. SCC can develop on the lips, tongue, and inside the mouth. Oral SCCs are often linked to HPV infection, heavy smoking, or alcohol use. Any sore or ulcer inside the mouth that has not healed within two to three weeks should be assessed by a specialist promptly, usually a maxillofacial surgeon or an ear, nose and throat specialist.
Is squamous cell carcinoma linked to sun damage earlier in life?
Yes. Cumulative UV exposure over a lifetime is the primary cause of SCC, and damage sustained during childhood and early adulthood contributes significantly to lifetime risk. This is why sun protection from an early age is so important, even if the effects of UV damage may not become apparent until decades later.