About Basal Cell Carcinoma (BCC)
Understanding BCC
About Basal Cell Carcinoma
If you have recently been diagnosed with basal cell carcinoma, or you are researching a suspicious lesion on your skin, the most important thing to know is this: basal cell carcinoma is the most common and most treatable form of skin cancer in the UK.
When it is caught and treated early by a specialist, the outlook is excellent. This article covers everything you need to know about BCC — what it is, what causes it, how it is diagnosed, and what your treatment options are.
Key Takeaways
- Basal cell carcinoma is the most common form of cancer in the UK, with around 147,000 new cases diagnosed every year
- It is the least aggressive type of skin cancer — it grows slowly and very rarely spreads to other parts of the body
- The primary cause is long-term UV exposure from sunlight or sunbeds, though genetics and other risk factors also play a role
- Common signs include a pearly or translucent bump, a flat scar-like patch, or a sore that bleeds and repeatedly fails to heal
- BCC will not resolve on its own — early treatment by a specialist is always simpler and leads to better outcomes
- Mohs micrographic surgery offers the highest cure rate of any BCC treatment — up to 99% for primary BCCs
- Risk can be significantly reduced with daily SPF 50+ sunscreen, protective clothing, and avoiding sunbeds entirely
The Most Common Skin Cancer
What Is Basal Cell Carcinoma?
Basal cell carcinoma (BCC) is a type of skin cancer that develops in the basal cells, which form the deepest layer of the outer skin (the epidermis). It is the most common cancer in the UK, more common than all other cancers combined, with around 147,000 new cases diagnosed every year.
BCC grows slowly and, in the vast majority of cases, stays localised to the area where it first appeared. It very rarely spreads to other parts of the body, which makes it the least aggressive form of skin cancer. That said, it will not resolve on its own and should always be seen by a specialist who will then help you arrive at a management plan that suits you.
There are several subtypes of BCC, each with a slightly different appearance and behaviour:
- Nodular BCC — the most common type, most often found on the face
- Superficial BCC — most common on the trunk and shoulders
- Morphoeic or Infiltrative (sclerosing) BCC — the most difficult to detect and treat
- Pigmented BCC — can resemble a melanoma due to its darker colouring
- Basosquamous BCC — the most aggressive subtype, requiring prompt treatment

Request an e-Consultation
Speak with Miss Rakhee Nayar from the comfort of your own home and receive expert advice on your skin concern, treatment options, and next steps.

Key Risk Factors for BCC
Causes & Risk Factors
The primary cause of BCC is cumulative exposure to ultraviolet (UV) radiation from sunlight or sunbeds. Over time, UV radiation damages the DNA in basal cells, which can cause them to multiply in an uncontrolled way.
Whilst consistent sun protection plays an important role in reducing your risk, some people develop BCC due to genetic factors that are outside of their control. If you fall into a higher risk group, regular skin checks are strongly recommended.
Several factors can increase your risk of developing BCC:
Sunbed use: artificial UV radiation carries the same risks as natural sunlight
A weakened immune system: including patients taking immunosuppressant medication
A history of sunburn: particularly severe sunburn during childhood
Certain inherited conditions: such as Gorlin syndrome, which significantly increases the risk of developing multiple BCCs
What Are the Symptoms of Basal Cell Carcinoma?
In its early stages, BCC does not usually cause pain, which is one of the reasons it can be easy to overlook. The most common signs to look out for include:
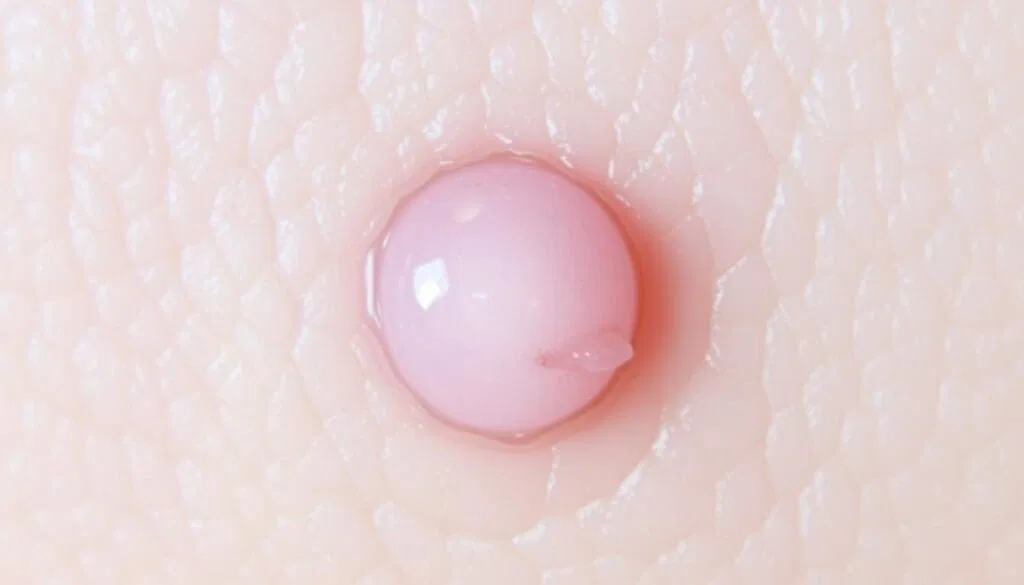
- A pearly, shiny, or translucent bump on the skin — often described as looking like a small pearl or an unusual pimple that never resolves
- A flat, scar-like patch without any history of injury to that area
- A pink or red scaly patch that resembles eczema or dry skin
- A sore that bleeds easily, crusts over, and repeatedly fails to heal fully
- Visible small blood vessels (telangiectasia) on or around the surface of the lesion

Symptoms Checklist
When checking your skin, the ABCDE checklist can be a helpful guide:
Border: edges are irregular, rolled, or poorly defined.
Diameter: any size warrants attention, particularly if growing.
Evolution: any change in size, shape, colour, or a new symptom such as bleeding or crusting.
How Is BCC Diagnosed?
If you or your GP suspects a BCC, you will be referred to a specialist for a clinical assessment. The specialist will examine the lesion carefully and, in most cases, perform a skin biopsy to confirm the diagnosis. This involves removing a small sample of tissue from the lesion, which is then examined under a microscope in a laboratory.
Biopsy results are typically available within one to two weeks. Further imaging is rarely required for BCC, as it seldom spreads beyond the skin. Once a diagnosis is confirmed, your specialist will discuss the most appropriate treatment options based on the size, location, subtype, and depth of your BCC.
The earlier a BCC is diagnosed, the simpler the treatment and the better the outcome. Always seek assessment promptly rather than monitoring a suspicious lesion at home.
- Large or deeply invasive
- Located on the ears or lips
- Poorly differentiated under the microscope
- Arising within scars or areas of chronic inflammation
- Occurring in patients with a weakened immune system
How Is Basal Cell Carcinoma Treated?
Treatment for BCC depends on several factors, including the subtype, size, location, and depth of the tumour. Your specialist will recommend the most appropriate approach for your individual circumstances.
Mohs Micrographic Surgery
The gold-standard treatment for BCC, offering the highest cure rate of any available technique. Particularly recommended for facial BCCs and high-risk subtypes.
Surgical Excision
The lesion is cut out with a small margin of healthy surrounding tissue and the wound is neatly closed with sutures. A straightforward and widely used option for many BCCs in lower-risk locations.
Curettage & Cautery
The lesion is scraped away and the wound sealed using heat. Used for superficial BCCs in low-risk areas and achieves cure rates of close to 95%.
Radiotherapy
A non-surgical option used when a patient is not suitable for surgery, for example due to age or an underlying medical condition.
Topical Treatments
Prescription creams such as imiquimod or 5-fluorouracil are applied directly to the skin. Suitable only for small, superficial BCCs and achieve cure rates of between 80 and 90%.
Mohs Surgery for Basal Cell Carcinoma
Mohs micrographic surgery is widely regarded as the most effective treatment available for basal cell carcinoma, particularly for lesions on or near the face. The procedure involves removing the tumour layer by layer, with each layer examined under a microscope in real time. This continues until no cancer cells remain, ensuring the complete removal of the tumour whilst preserving as much healthy surrounding tissue as possible.
The benefits of Mohs surgery for BCC include:
- The highest cure rate of any BCC treatment
- Maximum tissue preservation — particularly important around the eyes, nose, ears, and lips where every millimetre of healthy skin matters
- Immediate confirmation of clear margins — results are confirmed during the procedure itself, with no waiting for laboratory results
- Reconstruction performed in the same session — the surgical defect is repaired immediately, with no need for a separate procedure or a second surgeon

Consultant Plastic Surgeon
Miss Rakhee Nayar - One of the UK's Leading Mohs Surgeons
Miss Rakhee Nayar is one of the UK’s foremost specialists in Mohs micrographic surgery, bringing a rare combination of oncological precision and aesthetic expertise to the treatment of basal cell carcinoma. In a specialty where only 17% of consultants are women, she offers a uniquely compassionate and relatable perspective — particularly valued by her female patient base.
"My approach seamlessly combines rigorous oncological safety with deeply compassionate, individualised care."
One of fewer than 10 women in the UK dual-trained in plastic surgery and Mohs micrographic surgery
20+ years of surgical experience and a 99.9% patient satisfaction rate
MBChB with Honours, MRCS, FRCS Plast, and MD (Doctorate in Cancer Studies)
European Hand Diploma (EBHS) — unique ability to perform Mohs surgery on the hand
National Chairwoman for Mohs Training, Trainee Interface Group (TIG) — since January 2024
Member of BAPRAS, the Royal College of Surgeons of Edinburgh, BMA, CBS, and the British Society for Mohs Surgery
Can BCC Be Prevented?
Not all BCCs can be prevented, as genetic factors play a role for some patients. However, the risk of developing BCC can be significantly reduced with consistent sun protection habits.
Early detection is just as important as prevention. The sooner a BCC is identified and treated, the simpler the procedure required and the better the long-term outcome.
- Apply SPF 50+ sunscreen to all exposed skin every day, even during winter or overcast weather
- Wear protective clothing, including a wide-brimmed hat, in strong sunlight
- Avoid sunbeds entirely — there is no safe level of artificial UV exposure
- Seek shade during peak UV hours, between 11am and 3pm
- Check your skin regularly using the ABCDE checklist and seek prompt assessment of any changes
- If you are in a high-risk group, consider an annual skin check with a specialist


07740 306144
Frequently Asked Questions
Helpful Answers About BCC
Is basal cell carcinoma the same as skin cancer?
Yes. Basal cell carcinoma is a form of skin cancer, but it is the least aggressive type. It develops in the basal cells of the epidermis, grows slowly, and very rarely spreads to other parts of the body. With prompt specialist treatment, the vast majority of patients make a full recovery.
Can basal cell carcinoma go away on its own?
No. BCC will not resolve without treatment. Whilst it grows slowly, it will continue to grow and cause increasing damage to the surrounding skin and tissue if left untreated. Early treatment is always simpler and leads to better outcomes.
How quickly does BCC grow?
BCC typically grows slowly — often over months or years. However, the rate of growth varies between individuals and subtypes. Morphoeic and basosquamous BCCs tend to be more aggressive than nodular or superficial types. Any lesion that appears to be growing should be assessed promptly.
Is BCC hereditary?
BCC is not directly inherited in most cases, but a family history of skin cancer does increase your risk. Certain inherited conditions, such as Gorlin syndrome, are associated with a significantly higher risk of developing multiple BCCs. If skin cancer runs in your family, regular skin checks are strongly recommended.
Can BCC come back after treatment?
Recurrence is possible, particularly if the tumour was not fully removed during the initial procedure. This is why treatment by an experienced specialist using a technique with a high cure rate is so important. Mohs micrographic surgery offers the lowest recurrence rates of any BCC treatment, with cure rates of up to 99% for primary BCCs.